Gluconeogenesis Definition
The literal meaning of Gluconeogenesis is GLUCO – glucose; NEO – new; GENESIS – creation. Thus Gluconeogenesis is a biochemical term that describes the synthesis of glucose or glycogen from substances which are not carbohydrates.
Gluconeogenesis is the procedure that generates the energy giving fuel ’ glucose’ from substances other than carbohydrates, which are stored in the body , when the carbohydrate substrates are not sufficiently available as in starvation or when they are of great demand as in intense physical exertion. [1,2,3,4]
Gluconeogenesis Pathway
Basically Gluconeogenesis is the reversal of Glycolysis which is the process of breaking down of glucose to produce energy. [1]Glycolysis proceeds to another energy cycle called Citric acid cycle by forming a substance called pyruvate. So, Gluconeogenesis is just the reversal of Glycolysis – starting with pyruvate.
The substrates get converted to pyruvate or other intermediates of the Citric acid cycle by various chemical reactions from which Gluconeogenesis begins.
Which way does the process go if all the set of enzymes are same for both glucose synthesis and breakdown? This conflict is overcome by the 3 key steps in Gluconeogenesis which cannot occur with enzymes of Glycolysis.
So these 3 steps are circumvented by another set of enzymes to form glucose at the end.
Substrates of Gluconeogenesis
- Glucogenic amino acids like alanine and glutamine
- Lactate which is produced as a byproduct of glycolysis in muscles, red blood cells etc
- Glycerol, which is a part of triacylglecerol molecule in adipose tissue
- Fatty acid
- Citric acid cycle intermediates through oxaloacetic acid
Glucogenic amino acids
Glucogenic amino acid undergoes transamination which causes change in the carbon skeleton and directly gets converted to pyruvate. Some Glucogenic amino acids form oxaloacetic acid or other intermediates of Citric acid cycle. While alanine is preferred in liver, glutamine is preferred in kidney.
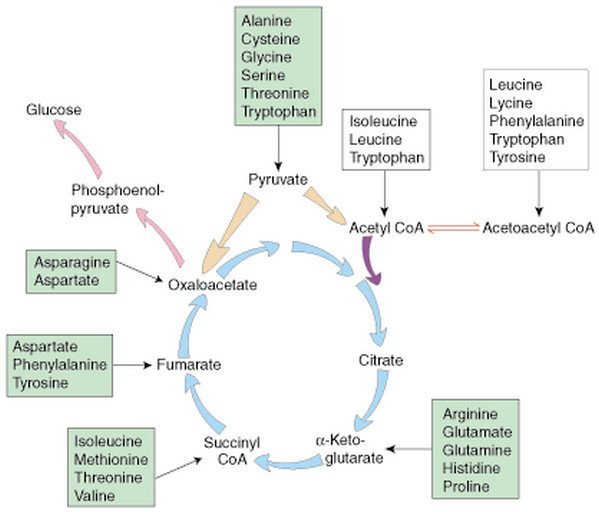
Picture 1: Conversion of Glucogenic amino acids to pyruvate
Image Source: img.sparknotes.com
Lactate
Muscular activities and anaerobic glycolysis in red blood cells produce a large amount of lactate. This lactate is taken up by the liver and gets converted to pyruvate by the enzyme lactate dehydrogenase.
Pyruvate then gets converted to glucose by hepatic Gluconeogenesis which is then sent back to muscles for reuse. This is known as Cori cycle [2, 5]

Picture 2: Cori cycle in liver
Glycerol
Glycerol is formed by breaking down of triacylglecerol in the fatty tissue. It is then carried to the liver where it gets converted to pyruvate and enters Gluconeogenesis. [8]
Gluconeogenesis steps:
- Gluconeogenesis starts either in mitochondria or cytoplasm through a series of enzymatically catalyzed steps. All the steps of Gluconeogenesis are the same as that of glycolysis with the same enzymes except in 3 steps. They are [1, 2]
- Glucose is converted to glucose 6 phosphate by glucokinase/ hexokinase in glycolysis which is reversed by glucose 6 phosphatase.
- Fructose 1 phosphate is converted to fructose 6 phosphate in glycolysis by phosphorfructokinase which is reversed by fructose 1, 6 bisphosphatase.
- Pyruvate is converted to phosphoenol pyruvate by pyruvate kinase in glycolysis and is reversed by pyruvate carboxylase and Phosphoenol pyruvate carboxy kinase.
- Rests are steps of Glycolysis in the opposite direction towards glucose using the same enzymes.
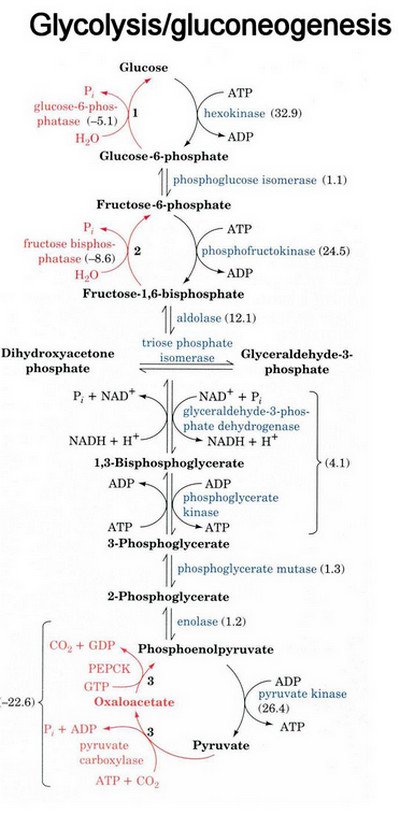
Picture 3: Steps of Gluconeogenesis
Image Source: isite.lps.org
Gluconeogenesis Enzymes
The enzymes that are same as that of glycolysis are
- Phosphoglucoisomerase
- Enolase
- Phosphoglycerate mutase
- Phosphoglycerate kinase
- G3P dehydrogenase
- Triosephosphate isomerase
- Fructose 1,6 bisphosphate aldolase
The key enzymes of Gluconeogenesis are
- Pyruvate carboxylase
- Phosphoenol pyruvate carboxykinase
- Fructose 1,6 bisphosphatase
- Glucose 6 phosphatase
Gluconeogenesis Regulation
Unlike the greedy human mind, the human body is built in such a way that when it senses the presence of a substance in excess, even the energy fuel like glucose, it triggers some mechanism to either utilize it or store it for future use.
When there is a scarcity of a substance, our body triggers some mechanisms which will either form the substance from other available chemicals or use an alternative source.
This is the basis of regulation. As Gluconeogenesis is the reversed process of glycolysis, both are regulated reciprocally. The factors which increase Glycolysis will decrease Gluconeogenesis and vice versa.
This regulation is needed to control the blood glucose level which will be either too low or too high in an unregulated condition. The regulation of this process is brought about by availability of substrates and through hormones. [3]
There are 3 types of regulation which takes place at different speed. They are
1. Change in the rate of enzyme synthesis – occurs over several hours
- Availability of substrate – Increased availability of Glucogenic amino acid stimulates Gluconeogenesis. High glucose increases the synthesis of enzymes of Glycolysis so that the glucose level is brought down. The opposite happens to the enzymes of Gluconeogenesis. The synthesis of gluconeogenic enzymes are decreased so that there is less formation of new glucose.
- Through hormones – Gluconeogenesis is increased by the Glucogenic hormones like glucagon, epinephrine and glucocorticoids. Glucagon stimulates phosphoenolpyruvate carboxykinase while insulin reduces the synthesis of these enzymes.
2. Covalent modification by reversible phosphorylation – rapid
- Phosphorylation is the process of addition of a phosphate group to an enzyme. On phosphorylation, some enzymes are activated while some are inactivated. The gluconeogenic hormones like glucagon and epinephrine leads to the phosphorylation of a key enzyme of glucose breakdown, pyruvate kinase which gets inactivated.
- This leads to inhibition of glycolysis and stimulation of Gluconeogenesis. This type of regulation acts as a rapid response to the presence of low glucose
3. Allosteric modification – instantaneous
- In addition to the enzymes that speeds up a reaction, other substances called allosteric activators further increase the rate of reaction. Acetyl coA is one such allosteric activator.
Acetyl coA in Gluconeogenesis:
In starvation, there is excessive breakdown of fatty acids resulting in formation of Acetyl coA in liver. They ensure the conversion of pyruvate to oxaloacetic acid. It acts as allosteric activator of the enzyme pyruvate carboxylase and inhibits pyruvate dehydrogenase of Glycolysis. [1]
It is inhibited by ADP and glucose. Thus Acetyl coA is sufficient to divert pyruvate into Gluconeogenesis from citric acid cycle. [8]
Important Hormones of Gluconeogenesis
The important hormones that regulate the blood sugar level and thus Gluconeogenesis are glucagon, insulin and glucocorticoids. The hormones which stimulate Gluconeogenesis and other mechanisms which increase the blood glucose level are called diabetogenic hormones.
Gluconeogenesis and Glucagon:
Glucagon is synthesized by alpha cells of pancreas. They stimulate the Gluconeogenesis by 3 mechanisms. They are
- When the glucose level is high, the key enzyme of Gluconeogenesis – fructose 1, 6 bisphosphatase is kept under check by its fructose 2, 6 bisphosphate. During fasting, glucagon inhibits the enzyme catalyzing the synthesis of fructose 2, 6 bisphosphate. This removes the inhibition on the key enzyme of Gluconeogenesis and stimulates it. Thus it acts as a counter hormone to insulin.
- It causes conversion of pyruvate kinase to its inactive form by phosphorylation thus inhibiting Glycolysis and favoring Gluconeogenesis.
- It increases the transcription of Phosphoenolpyruvate carboxykinase gene there by increasing the availability of the enzyme. [8]
Gluconeogenesis and Glucocorticoids
Glucocorticoids are synthesized in the kidney under stressful condition like starvation and intense exercise. Thus cortisol is stimulated by low blood sugar and increased demand.
They increase Gluconeogenesis by increasing the breakdown of Glucogenic amino acid. They increase Gluconeogenesis in kidney more than liver through a series of complicated biochemical steps.
Gluconeogenesis and Insulin:
It is the anti diabetic hormone synthesized by beta cells of pancreas and its main function is to lower the blood glucose level. Increased glucose level leads to increased production of ATP, the energy currency of our cells.
This ATP acts on potassium and calcium channel of the beta cells of pancreas and leads to release of insulin. Insulin inhibits Gluconeogenesis and causes glucose uptake by cells. Epinephrine inhibits insulin while glucagon stimulates insulin. [1]
It reduces both hepatic and renal Gluconeogenesis to equal extent. [10, 11]
Organs of Gluconeogenesis
The major tissues capable of synthesizing glucose are liver and kidney. Only they have the sufficient gluconeogenic enzyme activity and glucose 6 phosphatase activity to release glucose into circulation [10] It occurs in small intestine to a small extent in fasting state.[1,2,3]
Hepatic Gluconeogenesis – Gluconeogenesis in liver
Liver is the major site of Gluconeogenesis. [2, 3] During first 12 hrs of fasting, the glycogen reserve gets depleted dramatically and Gluconeogenesis increases by its regulatory mechanism as said above. [9] Liver primarily uses lactate, alanine [10] and glycerol.
Lactate gets converted to pyruvate by Cori cycle and then undergoes Gluconeogenesis in liver. Alanine gets converted to glucose by Glucose – Alanine cycle. Also acetyl coA is predominantly produced in liver which further increases Gluconeogenesis [7] Hepatic Gluconeogenesis decreases in condition causing acidosis.
Alcohol – Gluconeogenesis
Alcoholics have impaired Gluconeogenesis and are more prone to low blood sugar because the metabolism of alcohol by alcohol dehydrogenase and aldehyde dehydrogenase, forms chemical molecules which results in the diversion of the substrates of Gluconeogenesis to other pathways to lipid accumulation.
This results in the fatty liver in the alcoholics and more chances for hypoglycemic episodes [9]. Thus any disease condition damaging the liver will affect Gluconeogenesis.
Renal Gluconeogenesis – Gluconeogenesis in kidney
Earlier it was thought that, liver is the major organ of Gluconeogenesis under normal condition while kidney comes to play only when the body is in distress as in acidosis or prolonged starvation.
But this notion has been challenged by recent studies and is found that kidney is as important as liver in post absorptive human state. [10] Gluconeogenesis occurs in the outer tissue of kidney called the cortex [2].
It mainly uses lactate, glutamine and glycerol. [10] Lactate dehydrogenase, glucose 6 phosphatase and fructose 1, 6 bisphosphatase makes it possible for Gluconeogenesis to occur in kidney. [6] Renal Gluconeogenesis is greatly stimulated by glucocorticoids.
This helps to maintain the normal blood sugar in people with liver disease and contributes to excess glucose in diabetes type 1 and 2. It is increased by acidosis in contrast to hepatic Gluconeogenesis. It is suppressed by insulin as much as in the liver [10]
Gluconeogenesis Vs Glycogenolysis
| Gluconeogenesis | Glycogenolysis |
|---|---|
| Substrates are non carbohydrate substance like lactate and amino acids | Substrate is glycogen which is a complex carbohydrate |
| Occur in liver and kidney and a small extent in muscle. | Occur in liver and muscles |
| There are 4 key enzymes – Pyruvate carboxylase, Phosphoenol pyruvate carboxykinase, Fructose 1, 6 bisphosphatase and Glucose 6 phosphatase | Key enzyme is glycogen phosphorylase |
| Pyruvate is the first step | Glucose 6 phosphate is the first step |
Both Glycogenolysis and Gluconeogenesis results in the synthesis of glucose and the hormone regulation for both the process is the same.
Animation on Gluconeogenesis – link
Reference:
- Harper’s illustrated biochemistry 28/e Gluconeogenesis and regulation of blood glucose
- http://en.wikipedia.org/wiki/Gluconeogenesis
- http://www.rpi.edu/dept/bcbp/molbiochem/MBWeb/mb1/part2/gluconeo.htm
- http://www.encyclo.co.uk/define/Gluconeogenesis
- http://www.elmhurst.edu/~chm/vchembook/615coricycle.html
- Kidney enzymes of Gluconeogenesis, Glycogenesis, Glycolysis and direct oxidation Exp Biol Med (Maywood)
- http://www.ncbi.nlm.nih.gov/pubmed/9467236
- Lippincott illustrated biochemistry 2/e – intermediary metabolism – Gluconeogenesis
- Biochemistry notes – usmle step 1
- http://www.ncbi.nlm.nih.gov/pubmed/9467236
- http://www.medscape.com/viewarticle/812072_3
